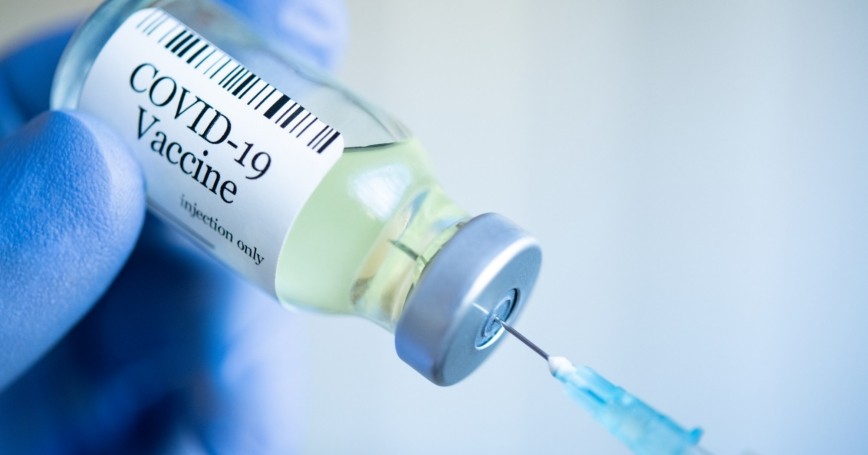
Vaccine, suspension of weakened, killed, or fragmented microorganisms or toxins, or other biological preparation, such as those consisting of antibodies, lymphocytes, or messenger RNA (mRNA), that is given primarily to prevent disease. A vaccine can confer active immunity against a specific harmful agent by stimulating the immune system to attack the agent. Once stimulated by a vaccine, antibody-producing cells called B cells (or B lymphocytes) remain sensitized and ready to respond to the agent should it ever enter the body.
A vaccine can also confer passive immunity by providing antibodies or lymphocytes already produced by an animal or human donor. Vaccines are usually given by injection (parenteral administration), but some are given orally or even through the nose (in the case of the flu vaccine). Vaccines applied to mucosal surfaces, such as those lining the gut or nasal passages, appear to stimulate a greater antibody response and maybe the most effective route of administration.
The first vaccinations
The first vaccine was introduced by British physician Edward Jenner, who in 1796 used the cowpox virus (vaccinia) to confer protection against smallpox, a related virus, in humans. However, before such use, Asian doctors applied the principle of vaccination and gave children dried scabs from the lesions of people suffering from smallpox to protect against the disease.
While some developed immunity, others developed the disease. Jenner’s contribution was to use a substance similar to, but safer than, smallpox to confer immunity. Thus, he took advantage of the relatively rare situation in which immunity to one virus confers protection against another viral disease. In 1881, French microbiologist Louis Pasteur demonstrated immunization against anthrax by injecting sheep with a preparation containing attenuated forms of the bacillus that causes the disease. Four years later he developed a protective suspension against rabies.
Vaccine effectiveness
After the time of Pasteur, an intensive and widespread search for new vaccines was carried out, and vaccines against bacteria and viruses, as well as vaccines against poisons and other toxins, were produced. Through vaccination, smallpox was eradicated worldwide in 1980 and polio cases were reduced by 99 per cent. Other examples of diseases for which vaccines have been developed include mumps, measles, typhoid, cholera, plague, tuberculosis, tularemia, pneumococcal infection, tetanus, influenza, yellow fever, hepatitis A, hepatitis B, some types of encephalitis, and typhus. although some of those vaccines are less than 100 per cent effective or are used only in high-risk populations. Vaccines against viruses provide particularly important immune protection because, unlike bacterial infections, viral infections do not respond to antibiotics.
Types of vaccines
The challenge in vaccine development is to design a vaccine strong enough to prevent infection without making the individual seriously ill. To that end, researchers have devised different types of vaccines. Weakened or attenuated vaccines consist of microorganisms that have lost the ability to cause serious disease but retain the ability to stimulate immunity. They can produce a mild or subclinical form of the disease. Attenuated vaccines include measles, mumps, polio (the Sabin vaccine), rubella, and tuberculosis. Inactivated vaccines are those that contain organisms that have been killed or inactivated with heat or chemicals.
Inactivated vaccines elicit an immune response, but the response is usually less complete than with live vaccines. Because inactivated vaccines are not as effective in fighting infections as those made with attenuated microorganisms, larger quantities of inactivated vaccines are administered. Vaccines against rabies, polio (the Salk vaccine), some forms of influenza, and cholera are made from inactivated microorganisms. Another type of vaccine is a subunit vaccine, which is made from proteins found on the surface of infectious agents. Influenza and hepatitis B vaccines are of that type. When toxins, the metabolic byproducts of infectious organisms, are inactivated to form toxoids, they can be used to boost immunity against tetanus, diphtheria, and whooping cough (whooping cough).
In the late 20th century, advances in laboratory techniques allowed for the refinement of approaches to vaccine development. Medical researchers could identify the genes of a pathogen (disease-causing microorganism) that code for the protein or proteins that stimulate the immune response to that organism. That allowed immune-stimulating proteins (called antigens) to be mass-produced and used in vaccines. It also made it possible to genetically alter pathogens and produce weakened strains of viruses. In this way, the harmful proteins of pathogens can be removed or modified, thus providing a safer and more effective method of manufacturing attenuated vaccines.
Recombinant DNA technology has also proven useful in developing vaccines against viruses that cannot be cultured successfully or are inherently dangerous. The genetic material that codes for the desired antigen is inserted into the attenuated form of a large virus, such as the vaccinia virus, which “piggybacks” the foreign genes. The altered virus is injected into an individual to stimulate the production of antibodies against foreign proteins and thus confer immunity. The approach potentially allows the vaccinia virus to function as a live vaccine against various diseases, once it has received genes derived from the relevant disease-causing microorganisms.
A similar procedure can be followed using a modified bacterium, such as Salmonella typhimurium, as the carrier of a foreign gene. Human papillomavirus (HPV) vaccines are made from virus-like particles (VLPs), which are prepared using recombinant technology. The vaccines do not contain live biological or genetic material from HPV and therefore cannot cause infection. Two types of HPV vaccines have been developed, including a bivalent HPV vaccine, made with VLPs of HPV types 16 and 18, and a quadrivalent vaccine, made with VLPs of HPV types 6, 11, 16 and 18.